Striking medical portraits show historical acne sufferers from the 19th century with their blemishes illustrated in vivid hues. Aisha Mazhar shares her reflections on these detailed depictions through her own experience of severe acne.
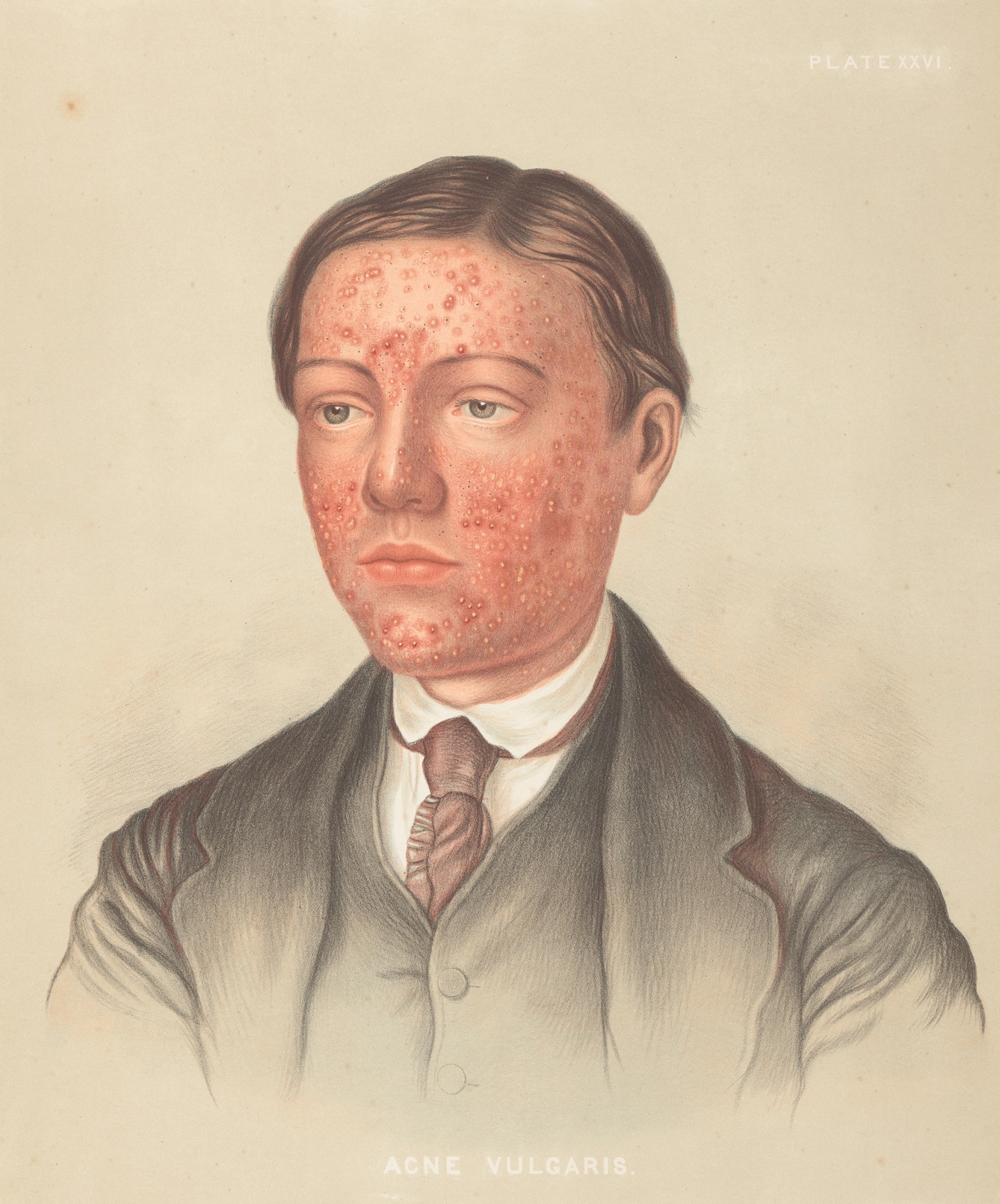
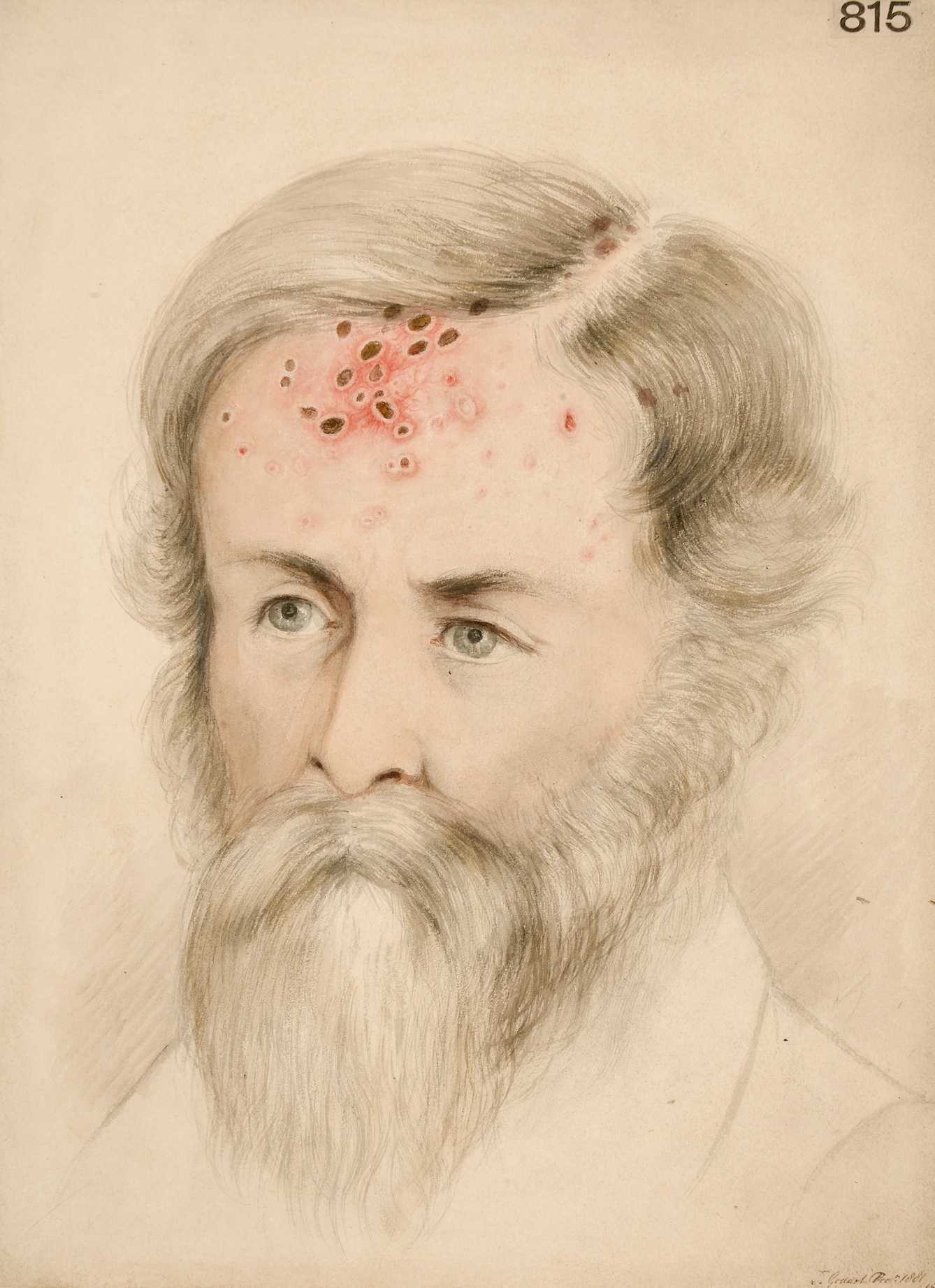
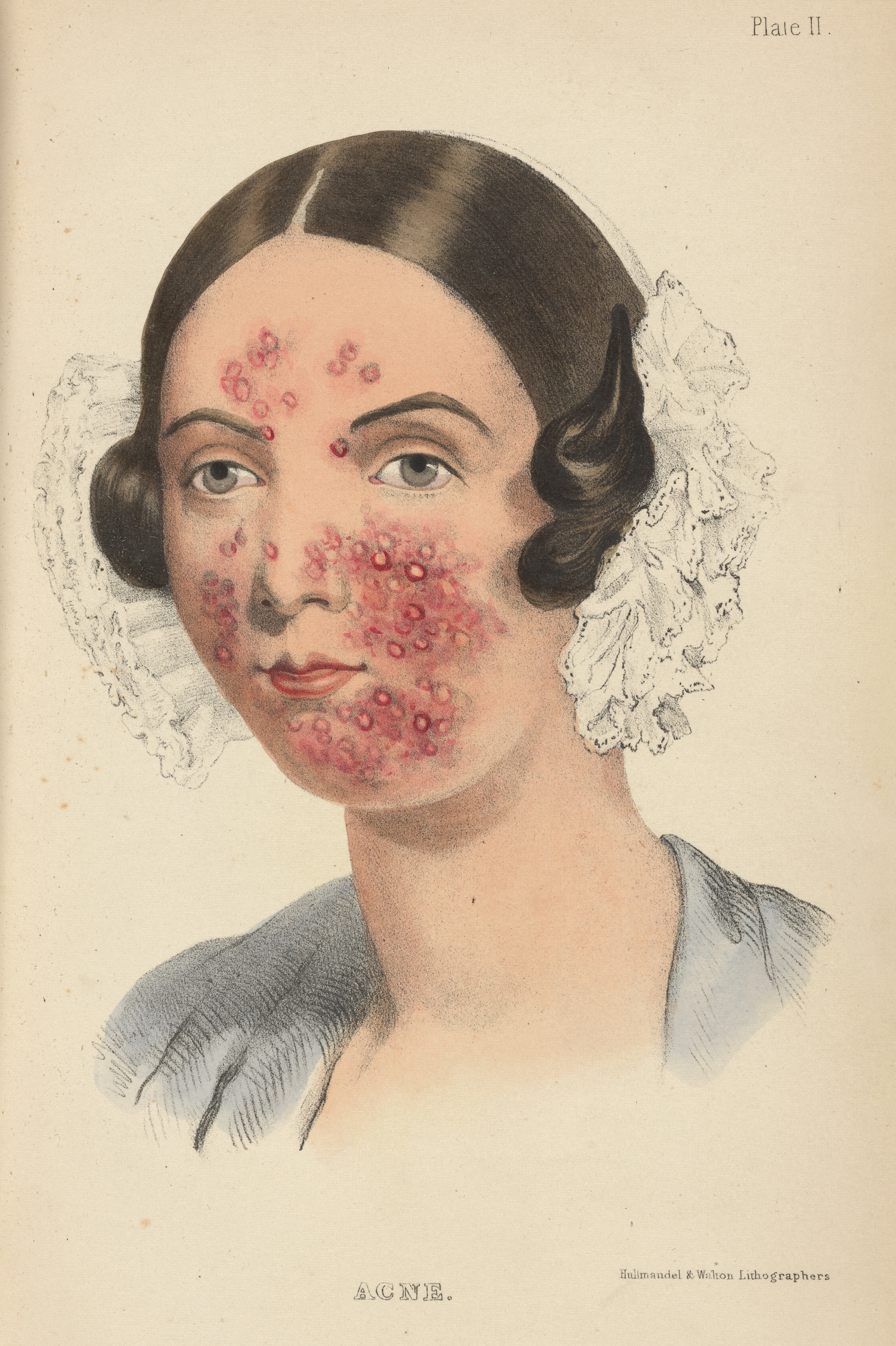
The first time I saw this portrait of a suited man, with his gaze averted and constellations of fiery pustules spread across his face, I couldn’t help but feel sympathy. It reminded me of my cystic acne, and the eight years I spent searching for an elusive ‘cure’ to alleviate my skin problems. I wonder if my historical counterparts depicted on the pages of dermatological texts were just as troubled by their skin.
Physicians like Jean-Louis Alibert produced coloured medical portraits of patients to characterise and distinguish skin conditions. They were used for teaching students or compiled into “skin atlases”, medical publications illustrating a variety of skin conditions, including acne. This reflected the increasing professionalisation of dermatology in the 19th century, as specialist skin hospitals were established in Britain and across Europe.
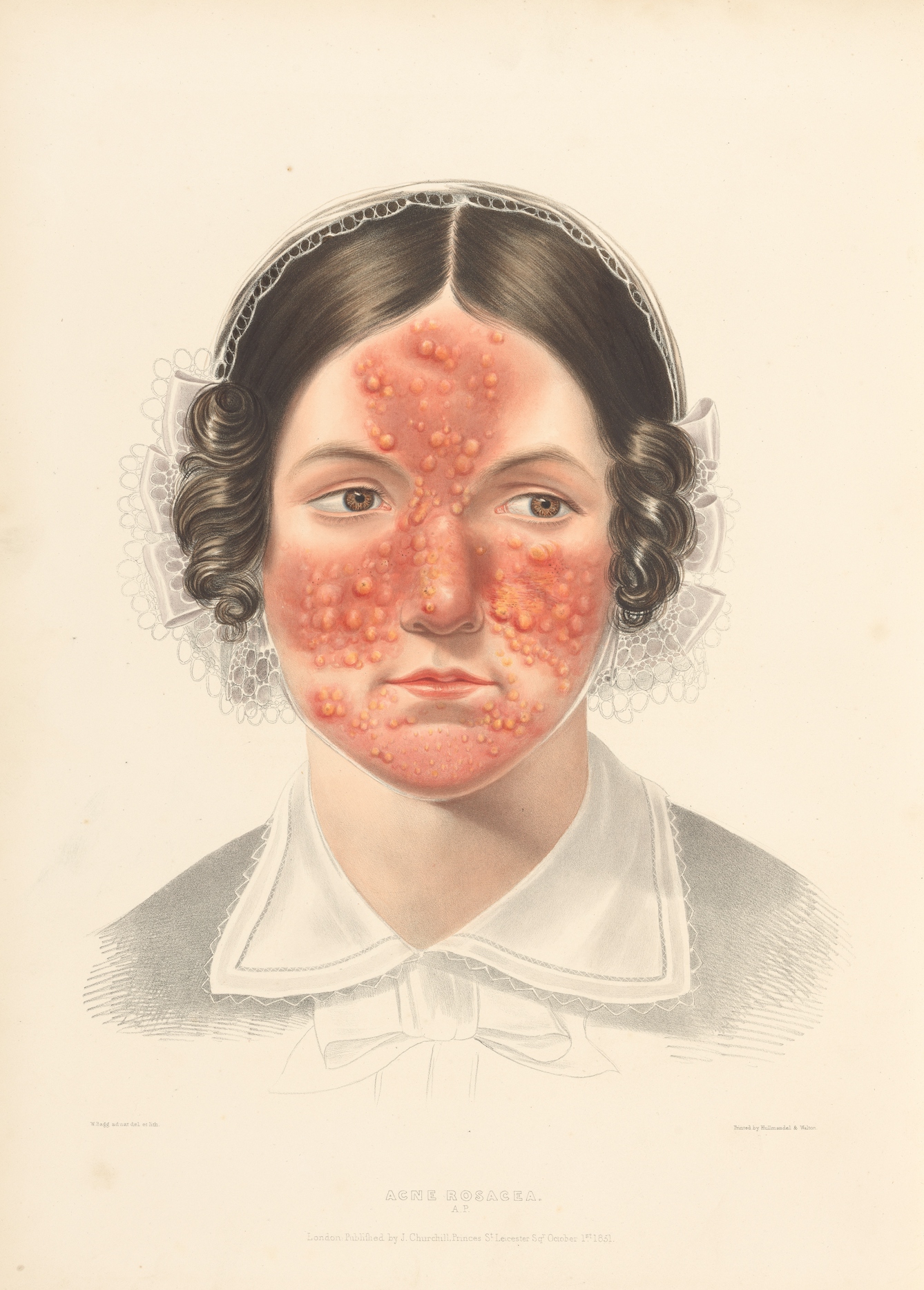
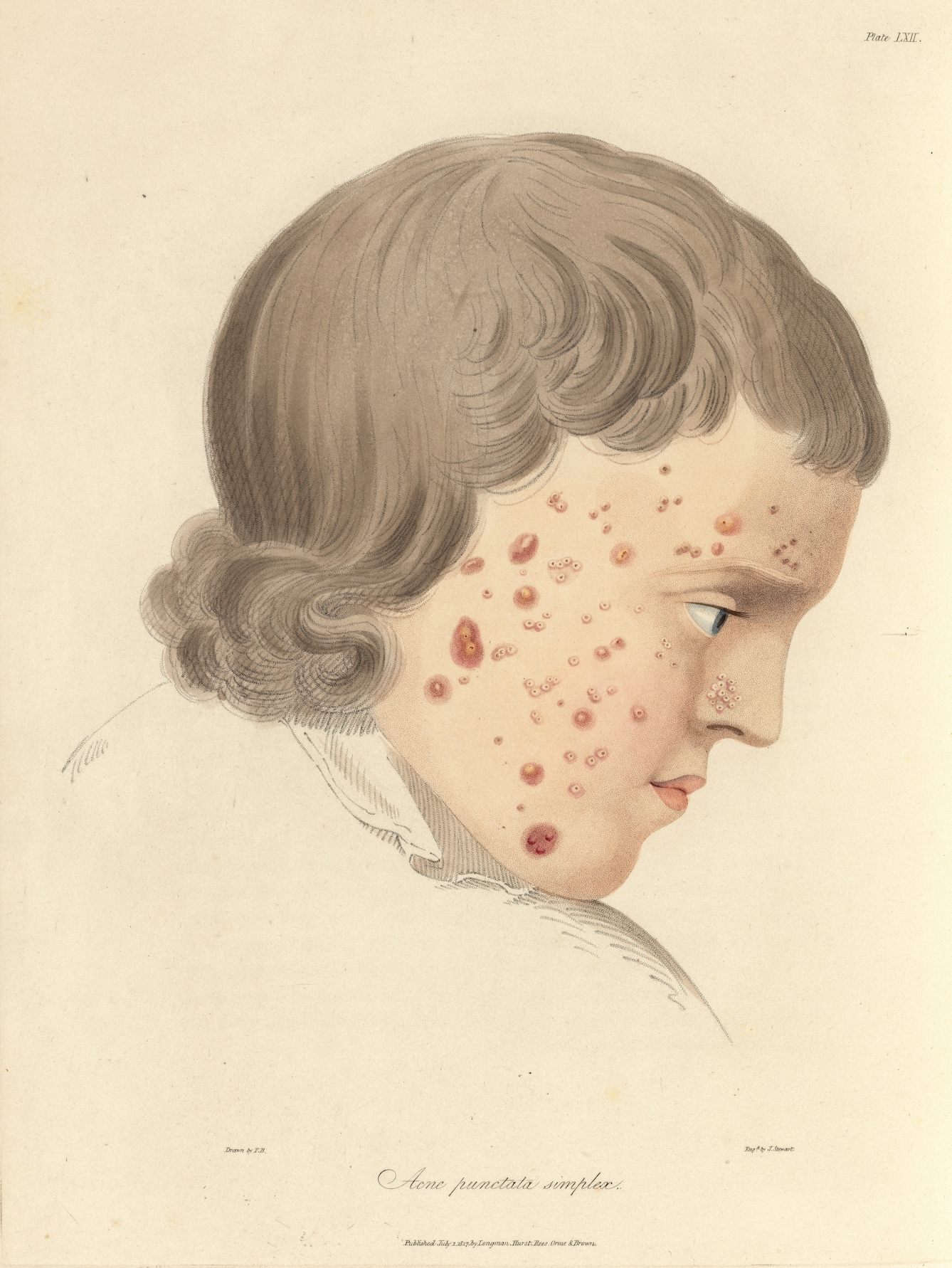
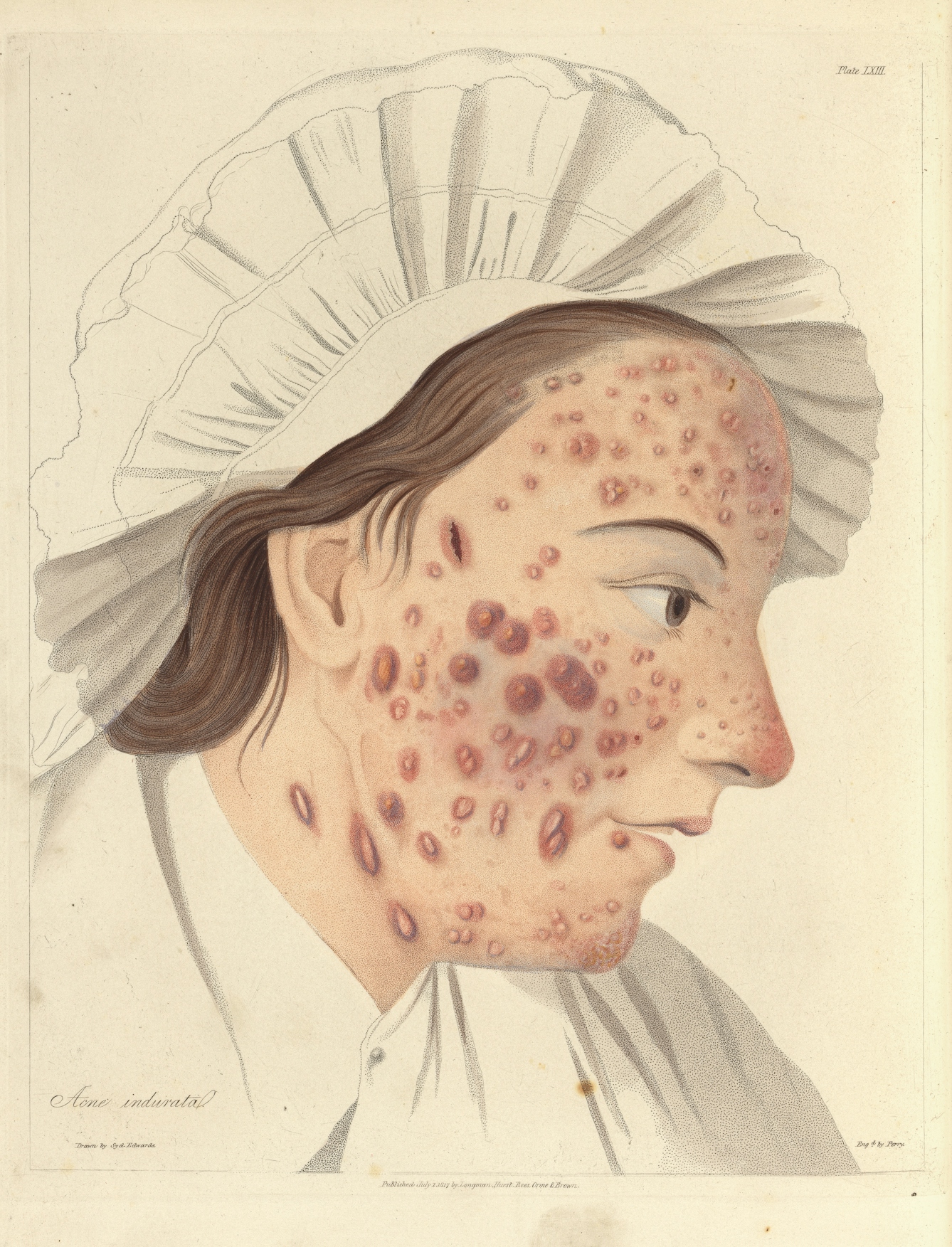
Portraits in skin atlases published by British physicians Robert Willan and Thomas Bateman formed part of their work to classify acne into four types: simplex, punctuate, indurate and rosacea, the last of which is now considered a separate skin condition. While we no longer differentiate acne as these four types, Willan and Bateman’s work demonstrates that acne was something physicians had to wrestle with; there was no easy fix.
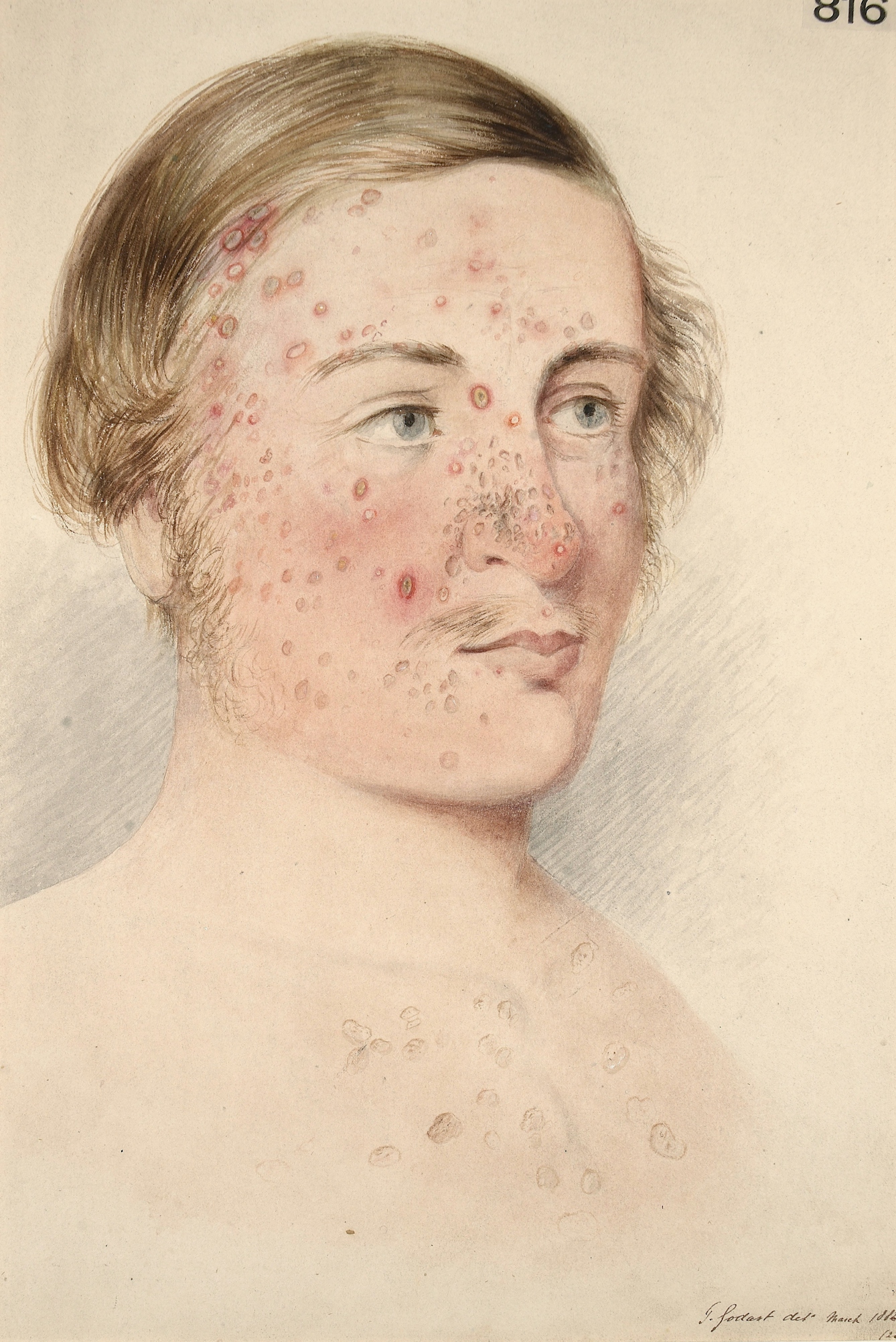
Many of the portraits were based on real people, while some were representations of a number of patients that physicians had encountered. Some portraits are accompanied by details of the subject, giving a tantalising glimpse into their lives. While there is information about their age, profession and the history of their skin condition, we are left to consider the psychological impact of their acne. My own relationship with my skin had a significant effect on my mental health and self-confidence. When my skin flared up, I felt reluctant to leave my bedroom.
Most of us will get the occasional pesky blemish, but when recurring blemishes are large and painful it can make dealing with it more fraught. The people in these portraits were proactively seeking medical help for their skin, which suggests it was causing them discomfort. I also turned to my GP several times in the hopes of finding a ‘cure’ for my stubborn acne, which showed no signs of abating, even as I approached my twenties.
Nineteenth-century acne treatments could include arsenic, or calomel pills made of mercury, which are both toxic substances. In the hope of alleviating their skin issues, acne sufferers were inadvertently poisoning themselves. While my search for a cure did not include toxic substances, I tried an exhausting array of skincare, home-made remedies, diets, and topical and oral medicine.
As our most visible organ, skin can attract judgement and comments. In the 19th century, clear skin became a visual marker of moral health to encourage public and private cleanliness at a time of frequent cholera outbreaks. With clear skin prized as an ideal, acne would have been an especially disconcerting condition to have.
I was often prompted to consider the importance of my complexion by the unsolicited advice and countless remedies that people would offer me. It was a constant reminder that my skin was a ‘problem’, a conspicuous one.
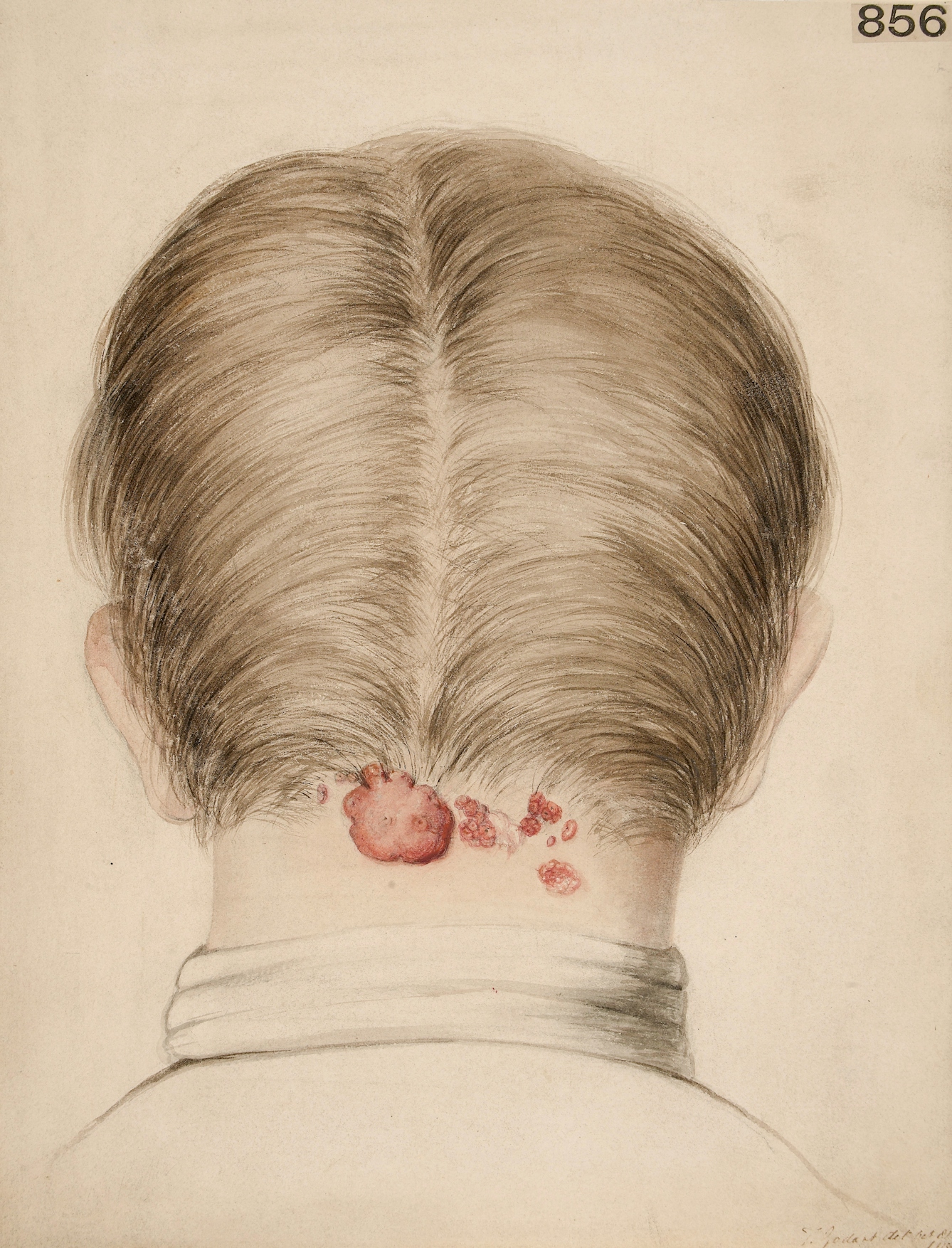
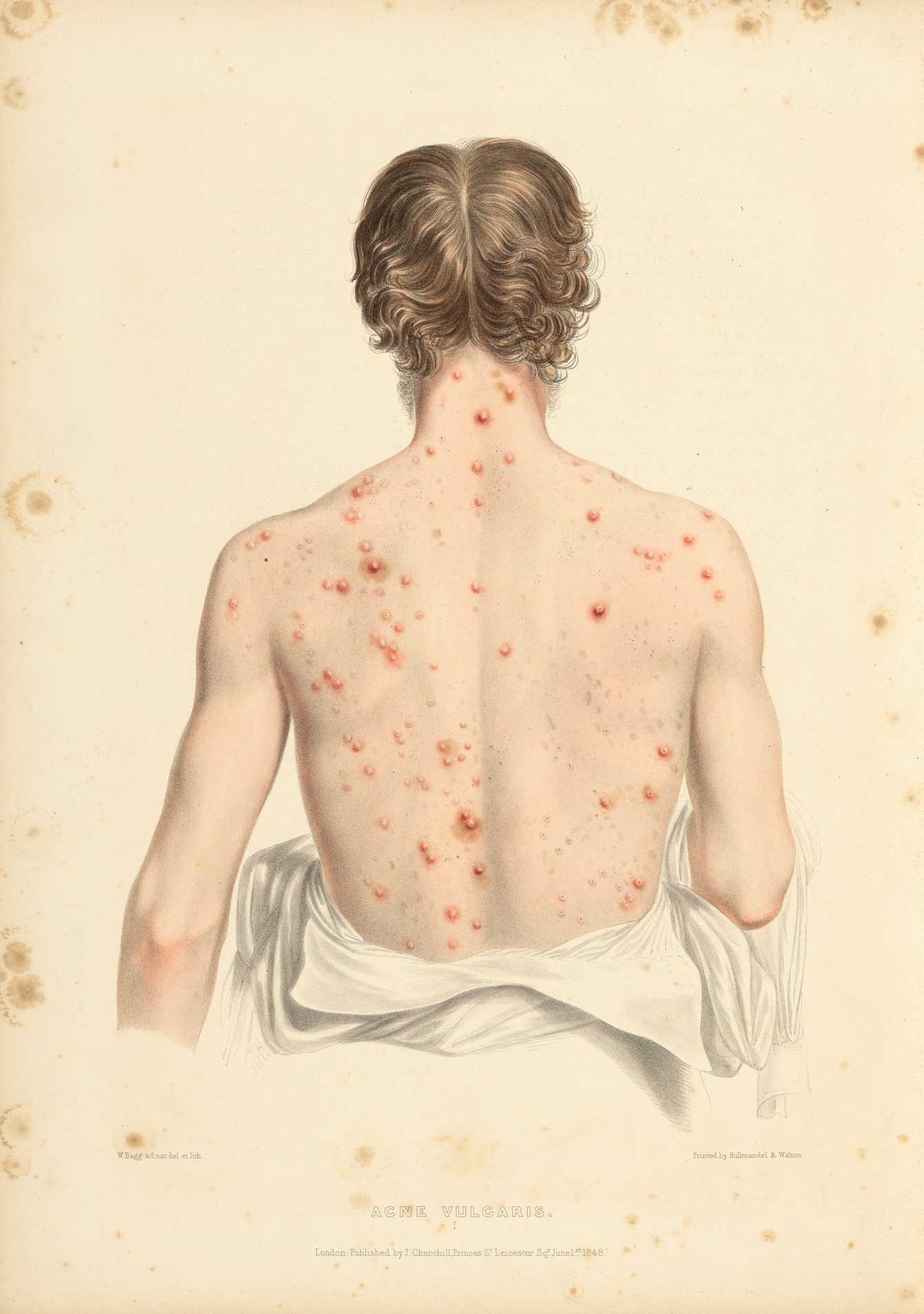
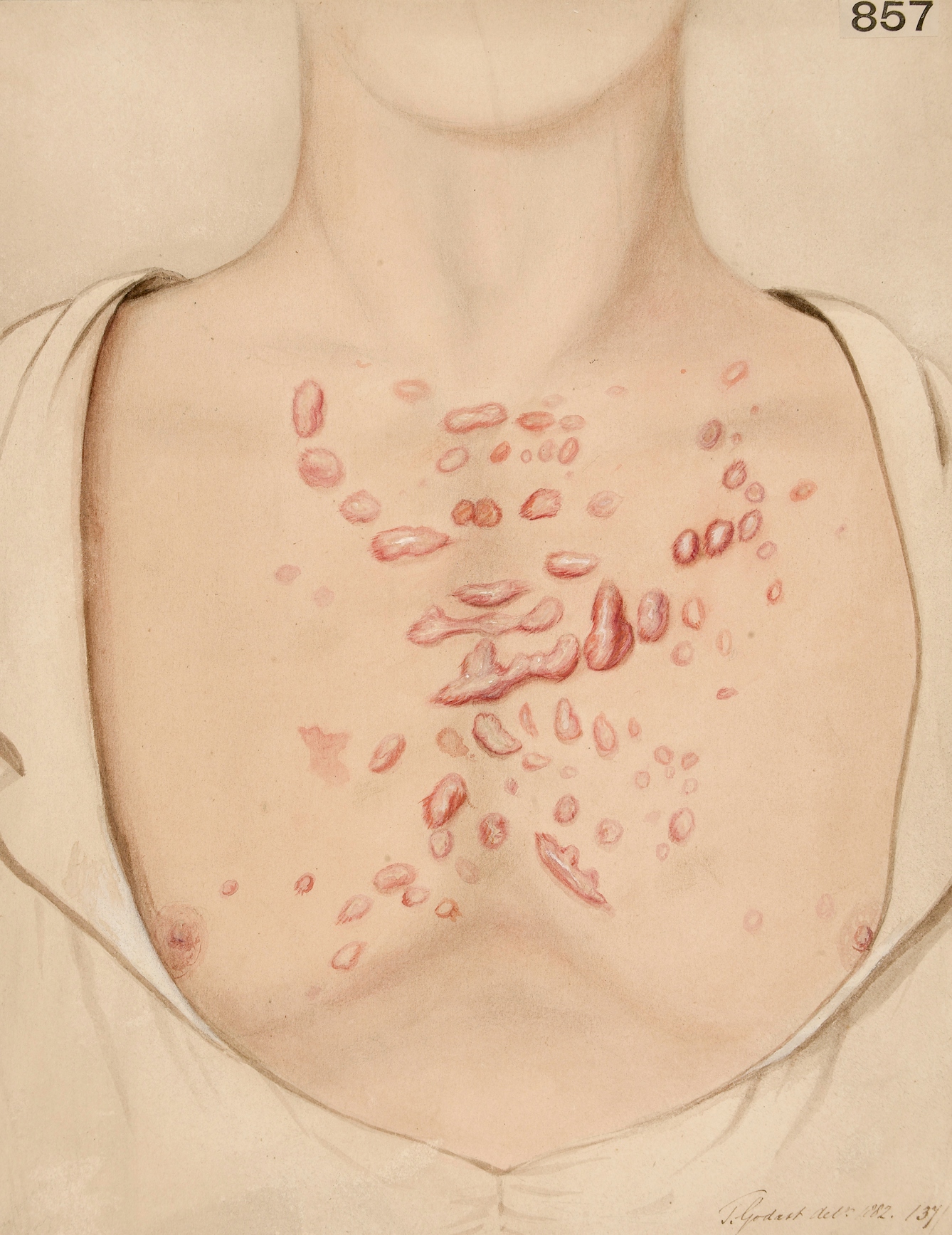
My acne wasn’t confined to my face: I was prone to blemishes on my shoulders and back. I would stand in front of a mirror, craning my neck to inspect each new painful arrival. My skin didn’t feel like my own: it felt like a constant invasion. I often wished that I could step out of my skin, into something less sore that wasn’t a patchwork of red.
At 21, I had one of my worst breakouts and turned up in tears at my doctor’s surgery. I was referred to a dermatologist, who prescribed me a six-month course of Roaccutane (isotretinoin). While it is an effective treatment, it is a drug mired in controversy. It can have serious side effects and requires regular blood tests, but for many like me, it can be life-changing.
Since taking Roaccutane, I no longer have acne. However, acne has left its mark through the keloid scars peppered across my shoulders. I also still worry that the acne will come back whenever I get the occasional blemish. For now, I am trying to savour being acne-free; it’s been a long journey to a finding a ‘cure’, after all. I hope that those historical acne sufferers found their cures too.
About the author
Aisha Mazhar
Aisha is a former graduate trainee at Wellcome. She has worked in science and health policy and is currently working for Arthritis UK.